What Is Endometriosis?
Everything You Need to Know About One of the Most Common and Most Misunderstood Conditions in Women's Health
Introduction :
A Disease That Has Been Waiting Too Long to Be Understood
Endometriosis affects an estimated one in ten women of reproductive age worldwide — more than 190 million women globally, making it more prevalent than diabetes and as common as asthma. It is responsible for up to 50% of cases of female infertility, accounts for a significant proportion of emergency gynecological admissions, and is one of the leading causes of chronic pelvic pain in women. And yet, despite its extraordinary prevalence and its profound impact on quality of life, the average woman with endometriosis waits seven to ten years before receiving a correct diagnosis.
This is not because endometriosis is rare. It is not because it is subtle. It is because it has been misunderstood, minimized, and consistently undertreated for generations. This article exists to change that — to give you the clear, honest, comprehensive information about endometriosis that you deserve to have from the very beginning of your journey.
What Is Endometriosis?
Endometriosis is a chronic, inflammatory, hormonal condition in which tissue similar to the lining of the uterus — called the endometrium — grows outside the uterus, in places where it does not belong. This misplaced tissue can be found on the ovaries, fallopian tubes, bowel, bladder, the lining of the pelvis, and in more advanced cases, on the diaphragm, the lungs, and other distant organs.
Every month, in response to the hormonal cycle, this misplaced tissue behaves exactly as the uterine lining does — it thickens, breaks down, and attempts to shed. But unlike the uterine lining, which exits the body during menstruation, the tissue outside the uterus has nowhere to go. It becomes trapped, causing inflammation, scarring, the formation of adhesions — internal scar tissue that can bind organs together — and in many cases, the development of cysts on the ovaries known as endometriomas, or chocolate cysts, named for the dark, old blood they contain.
It is important to understand that endometriosis is not an infection, not a cancer, and not contagious. It is a chronic condition that, while not life threatening in the conventional sense, can be profoundly life altering — affecting a woman's physical health, mental wellbeing, relationships, fertility, career, and overall quality of life in ways that are often invisible to the outside world.
What Causes Endometriosis?
Despite decades of research, the exact cause of endometriosis remains incompletely understood — a fact that reflects both the complexity of the disease and the historically inadequate level of research funding it has received relative to its prevalence. Several theories have been proposed, and it is likely that endometriosis results from a combination of factors rather than a single cause.
The most widely discussed theory is retrograde menstruation — the idea that during menstruation, some blood flows backward through the fallopian tubes into the pelvic cavity, depositing endometrial cells outside the uterus. While retrograde menstruation occurs in the majority of women, only a proportion develop endometriosis — suggesting that other factors, including immune system dysfunction, genetic predisposition, and hormonal influences, play an important role in determining who develops the disease and who does not.
Other theories include coelomic metaplasia — the transformation of cells lining the pelvis into endometriosis-like tissue — and lymphatic or vascular spread, which may explain the rare cases of endometriosis found in distant sites such as the lungs or brain. Genetic factors are clearly involved, as women with a first-degree relative with endometriosis have a significantly higher risk of developing the condition themselves. Environmental factors, including exposure to certain chemicals, have also been explored as potential contributors.
What is clear from the research is that estrogen is the primary hormonal driver of endometriosis — the disease grows in response to estrogen, which explains why it predominantly affects women of reproductive age and why hormonal therapies that reduce oestrogen levels are among the mainstays of medical management.
How Is Endometriosis Classified?
Endometriosis is classified in several ways — none of them perfect, and none of them universally adopted — reflecting the extraordinary complexity of a disease that refuses to fit neatly into any single categorization system.
The most widely known classification is the revised American Society for Reproductive Medicine staging system — commonly referred to as the rASRM stages I through IV, ranging from minimal to severe disease. This system scores endometriosis based on the location, extent, and depth of lesions, as well as the presence and severity of adhesions. While widely used, the rASRM system has significant limitations — most notably its poor correlation with pain symptoms. A woman with Stage I endometriosis can be in far more pain than a woman with Stage IV disease, and Stage IV disease does not necessarily mean worse fertility outcomes than Stage II. The system was designed primarily as a tool for predicting fertility outcomes rather than for guiding surgical planning or predicting pain — and its widespread use as a general severity classification has caused considerable confusion for patients and clinicians alike.
More recently, additional classification systems have been developed in an attempt to better capture the complexity of endometriosis — including the Enzian classification for deep infiltrating endometriosis and the Endometriosis Fertility Index for predicting fertility outcomes after surgery. Each system addresses some of the limitations of its predecessors while introducing limitations of its own. The absence of a single, universally adopted, clinically comprehensive classification system remains one of the field's most significant unsolved problems — contributing to inconsistencies in surgical planning, outcome reporting, and research methodology that ultimately disadvantage the patients these systems are meant to serve.
The Different Types of Endometriosis
Endometriosis is not one uniform disease — it presents in several distinct forms, each with its own pattern of symptoms, surgical challenges, and treatment implications.
Superficial Peritoneal Endometriosis:
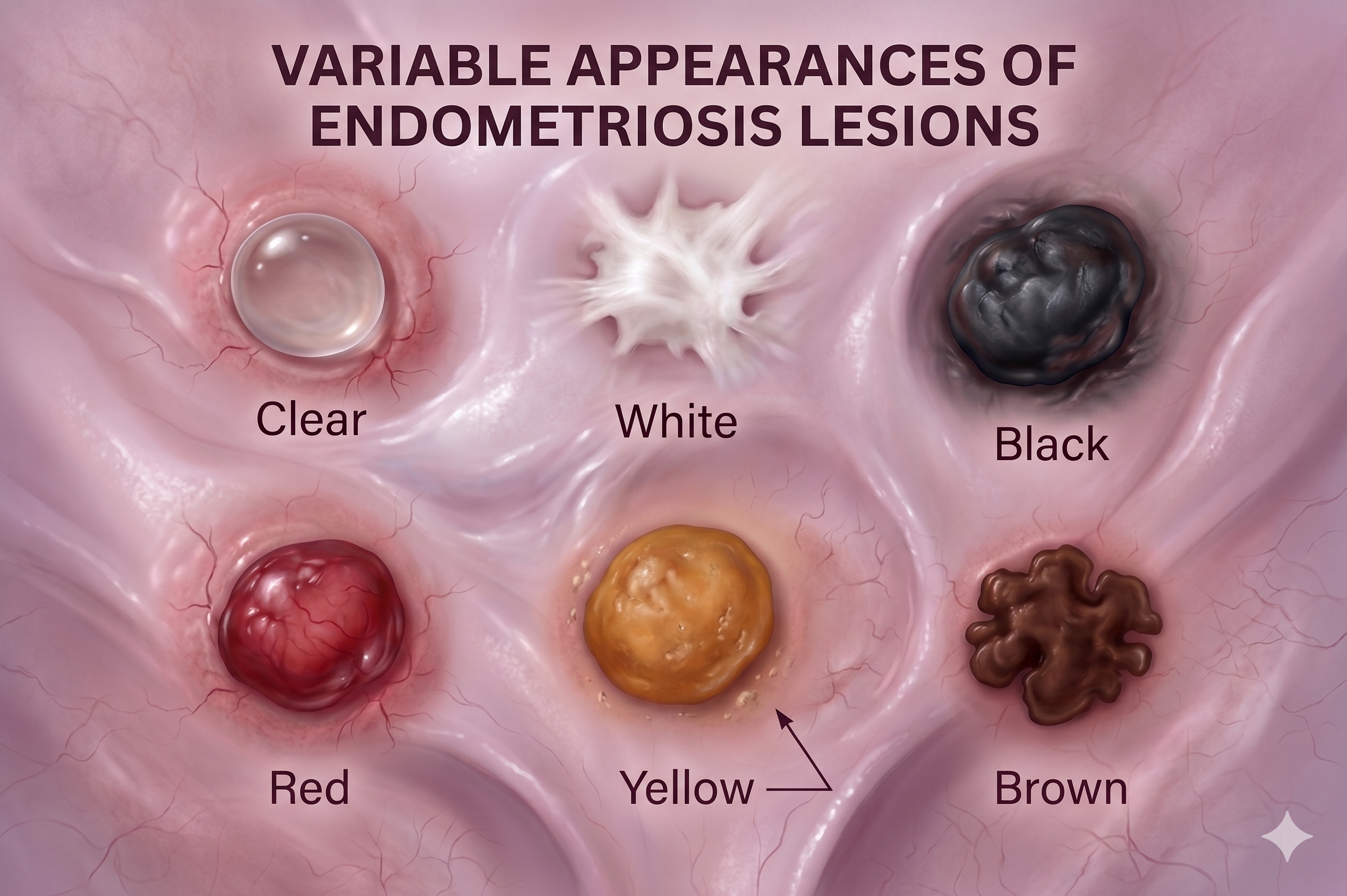
The most common form of endometriosis involves small lesions on the surface of the peritoneum — the thin membrane lining the inside of the pelvis and abdomen. These lesions can appear in a variety of colors — red, black, white, or clear — and their appearance can make them challenging to identify without specialist surgical training and experience. Despite being superficial, peritoneal lesions can cause significant pain through the inflammatory environment they create.
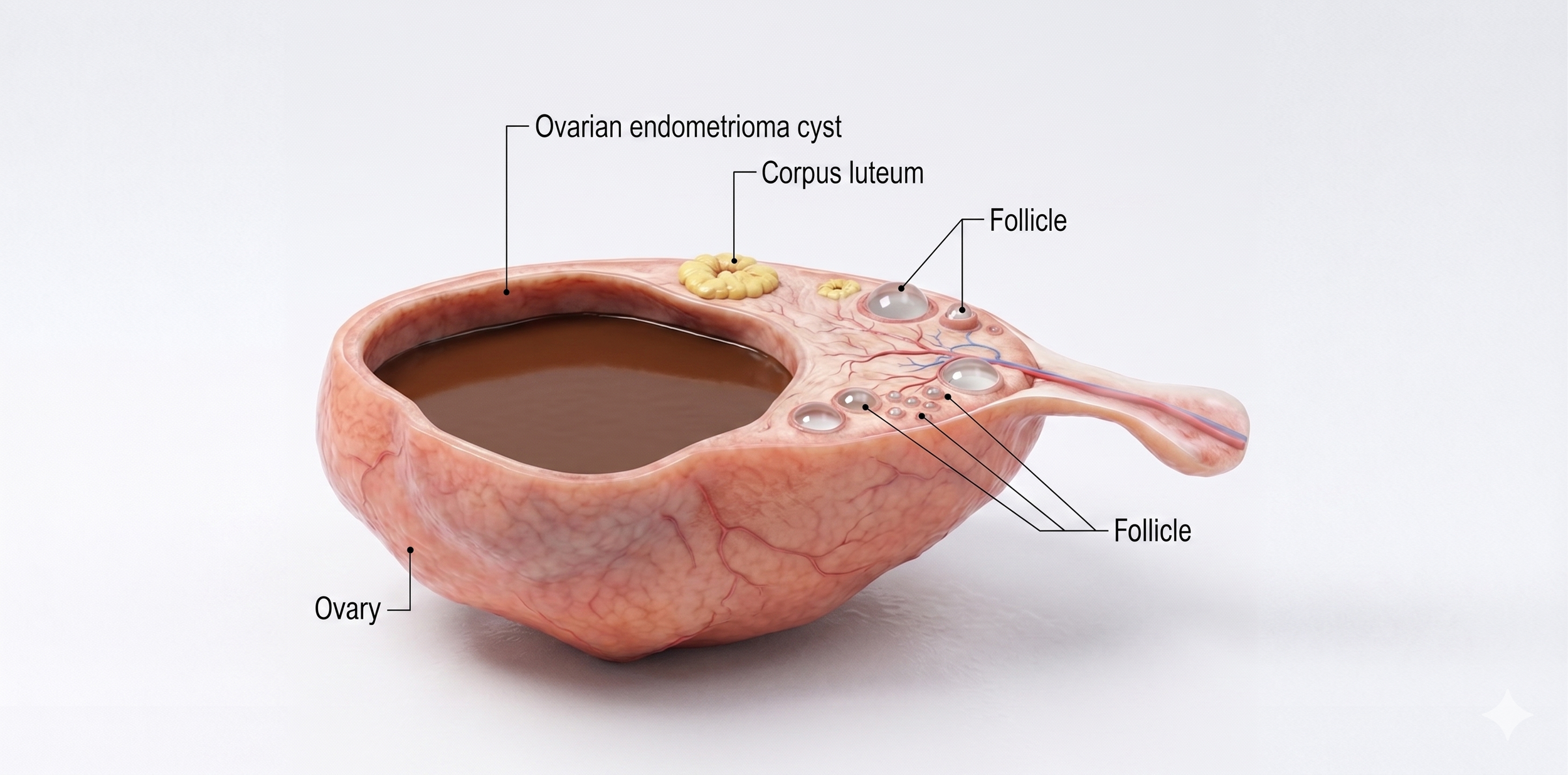
Ovarian Endometriosis : Endometriomas
When endometriosis involves the ovaries, it frequently forms cysts — endometriomas — filled with old, dark blood that has the appearance of liquid chocolate, giving rise to their common name of chocolate cysts. Endometriomas can grow to significant sizes, cause considerable pain, and have a well-documented damaging effect on the ovarian reserve — the pool of eggs available for future fertility. Complete surgical excision of endometriomas, rather than drainage or ablation, is associated with significantly lower recurrence rates and better long term outcomes.
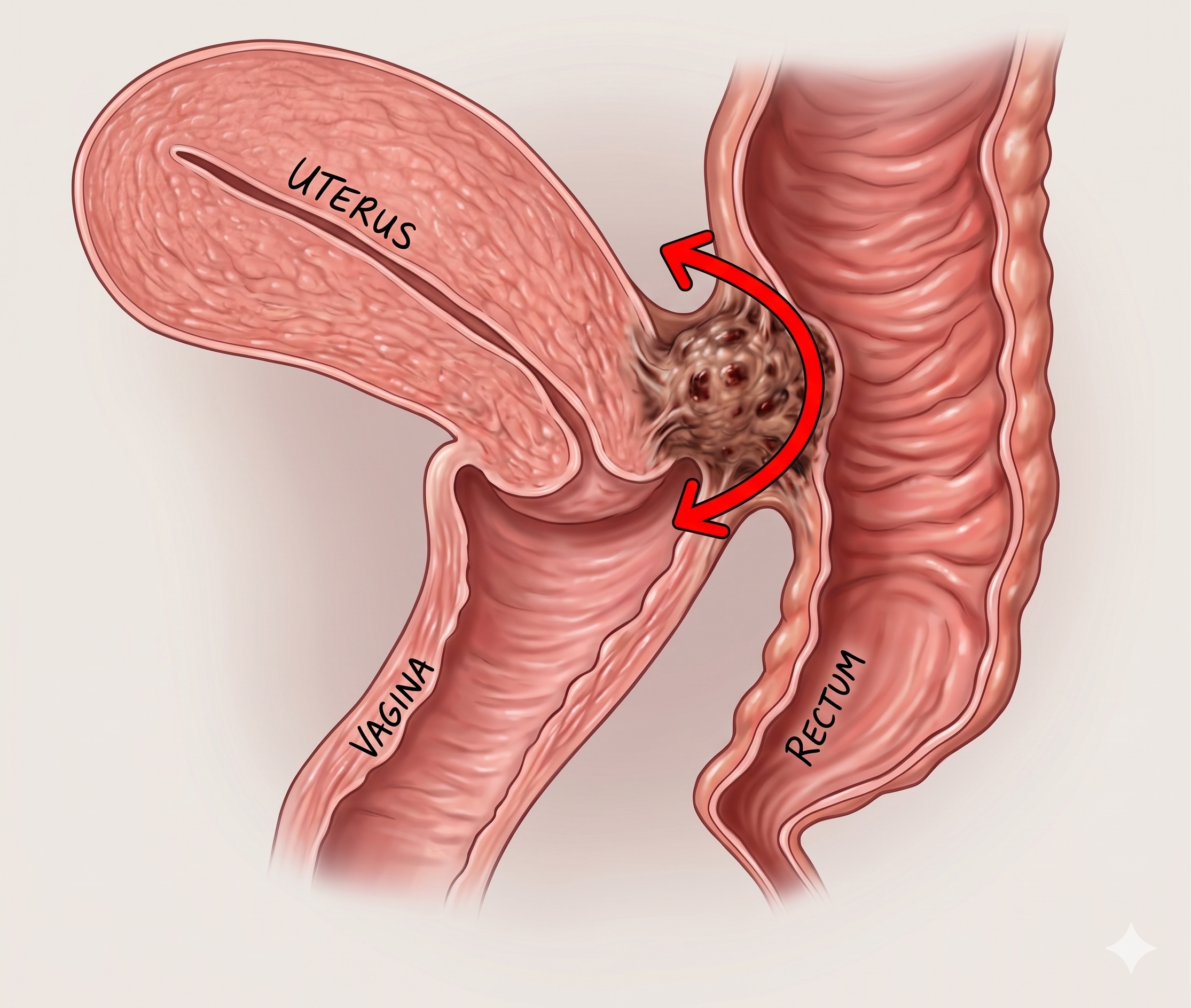
Deep Infiltrating Endometriosis:
Deep infiltrating endometriosis — defined as endometriosis that penetrates more than 5mm beneath the surface of affected tissues — is the most complex and surgically challenging form of the disease. It most commonly involves the uterosacral ligaments, the Pouch of Douglas, the bowel, the bladder, and the ureters. Deep infiltrating endometriosis is associated with the most severe pain symptoms and the greatest risk of organ damage — including silent ureteric obstruction that can progressively damage kidney function without causing obvious symptoms. Its surgical management requires a highly trained specialist and frequently a multidisciplinary operative team.