Diagnosing Endometriosis — From Symptoms to Imaging: What Every Woman Needs to Know
Understanding How Endometriosis Is Diagnosed — and Why Getting It Right From the Beginning Changes Everything
Introduction — The Diagnosis That Takes Too Long to Arrive
For most women with endometriosis, the diagnosis does not arrive quickly. It arrives after years — an average of seven to ten years — of painful periods dismissed as normal, symptoms attributed to irritable bowel syndrome, anxiety, or stress, and consultations that ended without answers. The diagnostic delay in endometriosis is not simply a medical inconvenience. It is a crisis — one that costs women years of their lives, allows disease to progress silently, and in many cases, permits irreversible damage to fertility and organ function before a single correct step is taken.
Understanding how endometriosis is diagnosed — what tools exist, what they can and cannot tell us, and what you have the right to ask for — is one of the most powerful things you can do at the beginning of your journey. This article will walk you through every dimension of endometriosis diagnosis, from the clinical symptoms that should raise immediate suspicion to the specialist imaging that can map the disease before surgery begins.
Clinical Diagnosis — When Symptoms Tell the Story
The Symptoms That Should Never Be Dismissed
Endometriosis diagnosis begins not in a scanning room or an operating theatre — it begins in a consultation room, with a clinician who is willing to listen carefully to what a woman describes about her own body. The clinical diagnosis of endometriosis is based on a constellation of symptoms that, taken together, paint a picture that should prompt immediate investigation rather than reassurance and discharge.
The symptoms that most strongly suggest endometriosis include deeply painful periods — medically known as dysmenorrhoea — that interfere with daily functioning and are not adequately controlled by standard over the counter painkillers. Chronic pelvic pain that persists beyond the menstrual cycle, pain during or after sexual intercourse — known as dyspareunia — painful bowel movements or urination particularly around the time of menstruation, significant bloating, and unexplained infertility are all symptoms that should prompt a clinician to consider endometriosis as a primary diagnosis rather than a last resort.
It is critically important to understand that the severity of symptoms does not reliably predict the severity of disease. A woman with minimal endometriosis can be in debilitating pain, while a woman with extensive deep infiltrating disease may have relatively subtle symptoms. This disconnect between symptom severity and disease extent is one of the most important and most frequently misunderstood aspects of endometriosis — and it means that no woman's symptoms should be minimised or dismissed simply because her pain seems disproportionate to what has been found so far.
Painful Periods Are Not Normal:
Perhaps the single most important clinical message in endometriosis diagnosis is one that has been dangerously normalised for generations — painful periods are not a normal part of being a woman. Mild cramping during menstruation is common and expected. But pain so severe that it prevents attendance at work or school, requires prescription strength analgesia, or leaves a woman unable to function for days every month is a medical symptom that demands investigation. Every clinician who dismisses severe period pain as normal is potentially delaying an endometriosis diagnosis by months or years — and every year of delay has consequences.
The Role of Clinical Examination:
A careful clinical examination — including a bimanual pelvic examination performed by an experienced clinician — can provide important diagnostic information. Tenderness on examination, particularly in the area behind the uterus, nodularity of the uterosacral ligaments, a fixed or retroverted uterus, or tenderness on movement of the cervix can all suggest the presence of endometriosis and should prompt further investigation. However, a normal pelvic examination does not exclude endometriosis — many women with significant disease have an entirely unremarkable examination, which is why imaging is an essential next step rather than an optional one.
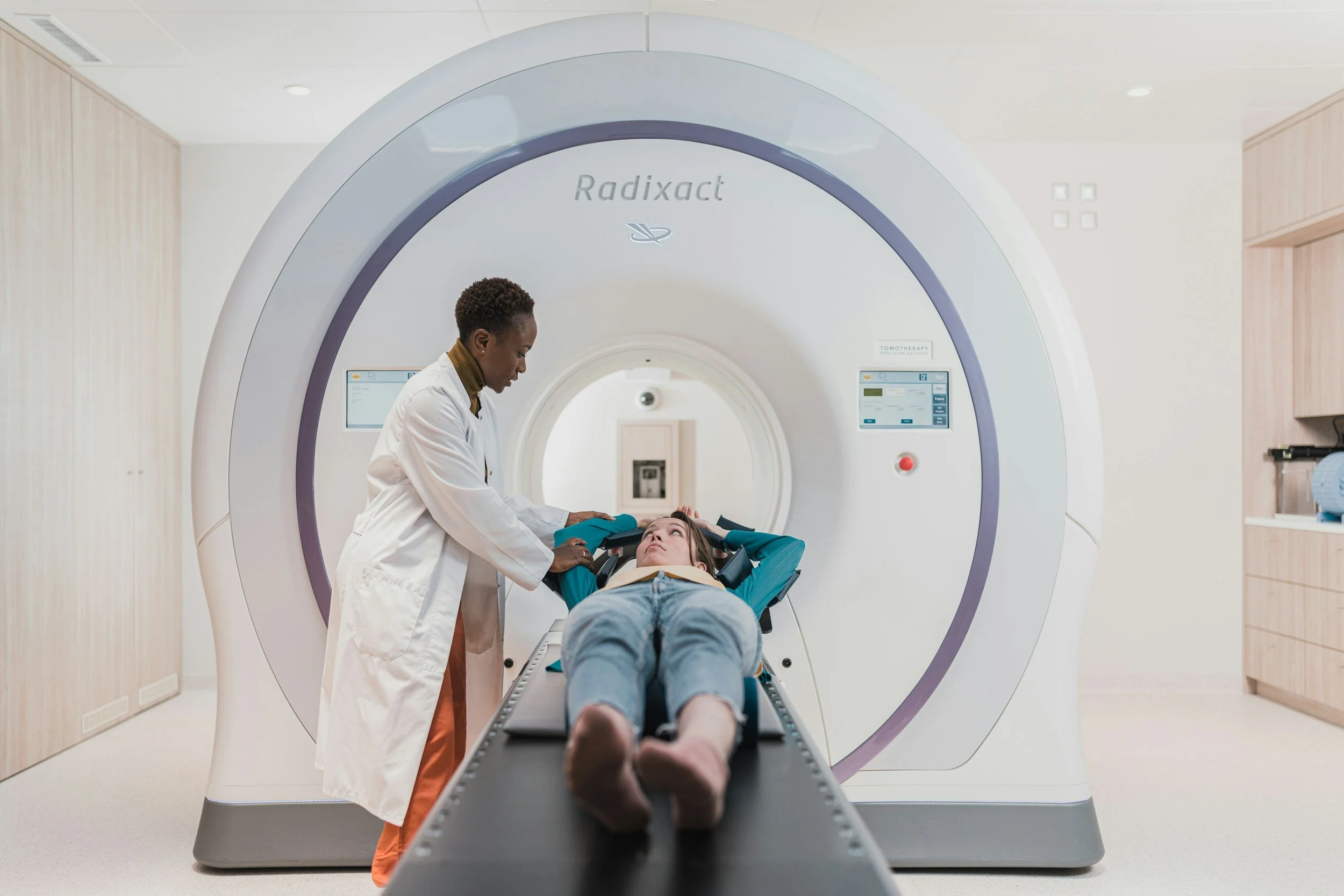
Imaging Based Diagnosis — Seeing the Disease Before Surgery
Why Imaging Matters — and Why Standard Scans Are Not Enough:
The advent of high quality specialist imaging has transformed the diagnosis of endometriosis — making it possible, in many cases, to identify, locate, and map the extent of disease without surgery. However, this transformation comes with a critically important caveat — endometriosis imaging is only as effective as the expertise of the person performing and interpreting it. A standard ultrasound or MRI performed without the endometriosis protocol, by a sonographer or radiologist without specific endometriosis training, will frequently miss the disease entirely — returning a falsely reassuring normal result that delays diagnosis and allows disease to progress.
This is perhaps the most dangerous misconception in endometriosis diagnosis — the belief that a normal scan means no endometriosis. A normal scan performed without specialist expertise means only one thing: that the person performing the scan did not find endometriosis. It does not mean that endometriosis is not there.
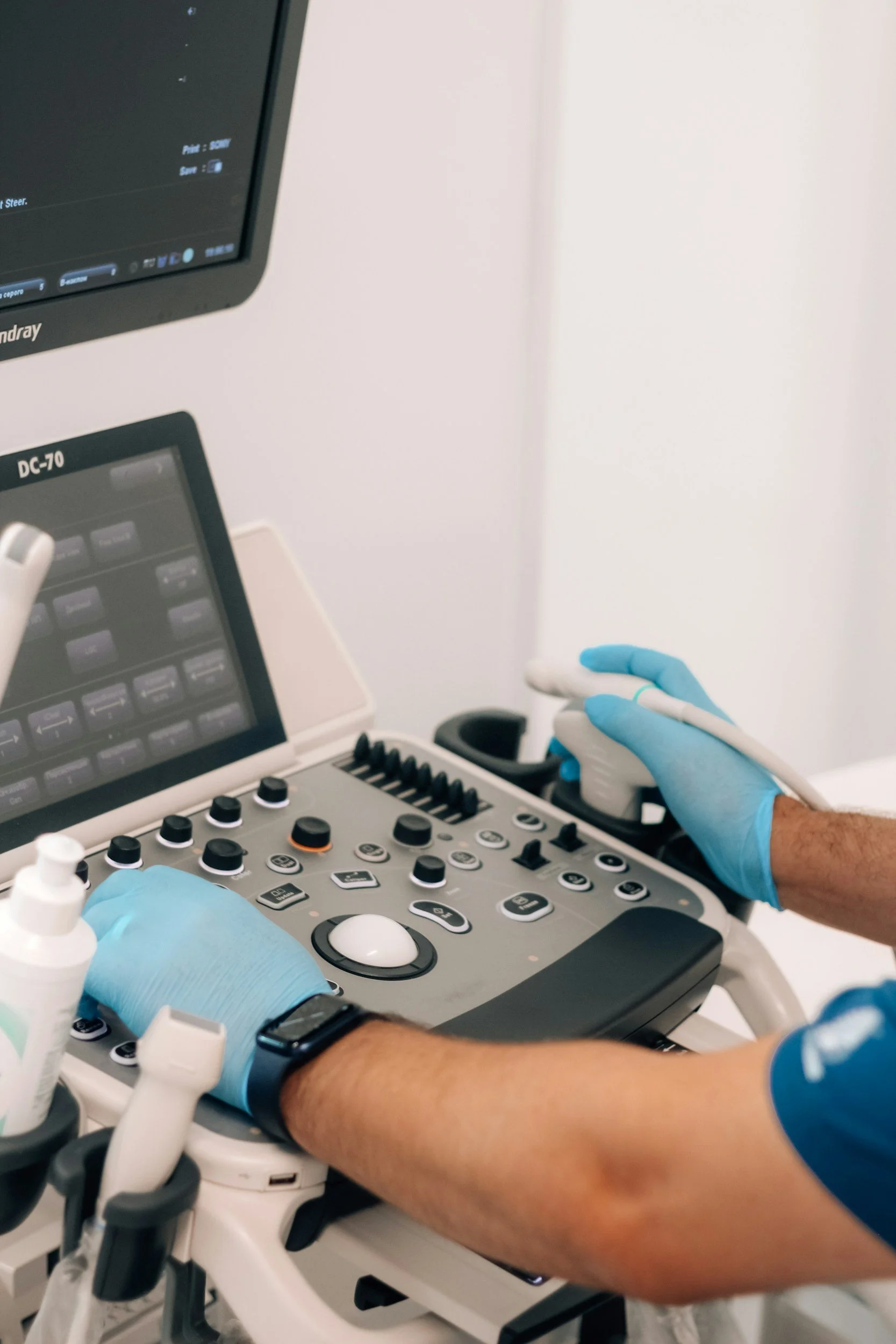
Transvaginal Ultrasound Under the Endometriosis Protocol:
The first line imaging investigation for suspected endometriosis is a transvaginal ultrasound performed under the endometriosis protocol — a structured, systematic examination of the pelvis conducted by a sonographer or gynecologist with specific training in endometriosis imaging.
This is fundamentally different from a routine pelvic ultrasound. Where a routine scan looks broadly at the uterus and ovaries, the endometriosis protocol ultrasound follows a detailed, systematic checklist that examines every potential site of endometriosis involvement, including the ovaries for endometriomas, the uterus for adenomyosis, the Pouch of Douglas for obliteration or deep disease, the bladder and its posterior wall, the bowel and rectosigmoid junction, the uterosacral ligaments, and the ureters.
A key and uniquely valuable technique used during this examination is the sliding sign — a dynamic assessment in which the examiner gently applies pressure with the probe to assess whether adjacent pelvic organs move freely against each other or are tethered by adhesions. Organs that slide freely indicate the absence of significant adhesive disease. Organs that do not slide — that are stuck to each other or to the pelvic wall — indicate the presence of adhesions, almost certainly caused by endometriosis, and provide critical information for surgical planning that no static image alone can offer.
When performed by an expert, transvaginal ultrasound under the endometriosis protocol has demonstrated high sensitivity and specificity for detecting ovarian endometriomas, deep infiltrating endometriosis of the bowel and bladder, and significant adhesive disease. It is the most accessible, most cost effective, and most immediately informative first line imaging investigation available — provided it is performed correctly, by the right hands.
MRI Under the Endometriosis Protocol:
For many patients — particularly those with suspected deep infiltrating endometriosis, complex disease involving multiple organ systems, or inconclusive ultrasound findings — a pelvic MRI performed under the endometriosis protocol is an essential complementary investigation. MRI uses magnetic fields to produce highly detailed images of soft tissue structures, offering a level of anatomical detail that ultrasound alone cannot always provide.
The endometriosis MRI protocol is a specialized sequence of images specifically designed to detect endometriosis deposits in their full extent and depth. When performed and interpreted by a radiologist with dedicated endometriosis training, it can identify deep infiltrating lesions involving the bowel wall, bladder, ureters, pelvic sidewall, and in advanced cases, the diaphragm and upper abdomen. It can assess the depth of bowel wall invasion — critical information for surgical planning — and identify ureteric involvement that may be causing silent kidney damage without obvious symptoms.
As with ultrasound, the critical factor is expertise. A standard MRI interpreted by a general radiologist without endometriosis specific training will miss a significant proportion of disease — particularly subtle deep infiltrating lesions and early adenomyosis. The protocol matters. The radiologist's training matters. And both are non-negotiable components of adequate endometriosis imaging.
When Is Laparoscopy Still Needed?
Despite the remarkable advances in specialist imaging, diagnostic laparoscopy — a minimally invasive surgical procedure in which a camera is inserted into the abdomen to directly visualise the pelvis — remains the gold standard for definitive diagnosis of endometriosis, particularly for superficial peritoneal disease that may not be visible on any imaging modality.
However, the role of laparoscopy in endometriosis diagnosis has evolved significantly. In the era of specialist imaging, laparoscopy is no longer simply a diagnostic tool — it should be simultaneously diagnostic and therapeutic, performed by a surgeon with the training and intention to excise all disease found at the time of surgery. A diagnostic laparoscopy that identifies endometriosis but does not remove it — leaving the patient to return for a second operation — represents a missed opportunity and an unnecessary additional surgical risk.
Furthermore, in patients with confirmed deep infiltrating endometriosis on specialist imaging, laparoscopy should never be a surprise encounter with the extent of disease. The imaging should have already told the surgeon what to expect — and the surgical team should have planned accordingly, with all necessary specialists present and prepared before the first incision is made.
The Diagnostic Delay — Why It Happens and What You Can Do
The seven to ten year average diagnostic delay in endometriosis is driven by a combination of factors that operate at every level of the healthcare system — from the societal normalization of period pain, to insufficient clinician training in endometriosis recognition, to the widespread unavailability of specialist imaging outside major centres.
As a patient, the most powerful tools available to you are knowledge and advocacy. Know that severe period pain is not normal and deserves investigation. Know that a normal standard scan does not exclude endometriosis. Know that you have the right to request imaging performed under the endometriosis protocol, by someone with specialist training. Know that a clinical diagnosis based on your symptoms alone is sufficient to justify specialist referral — you do not need to have failed every other treatment first.
And know that the right diagnosis, reached through the right pathway, by the right specialist — changes everything that follows.
Key Takeaways
The average diagnostic delay for endometriosis remains seven to ten years — driven by normalisation of symptoms and inadequate imaging
Clinical diagnosis is based on a constellation of symptoms including painful periods, pelvic pain, painful sex, bowel and bladder symptoms, and infertility
Severe period pain is never normal and always deserves investigation
A normal standard scan does not exclude endometriosis — specialist imaging under the endometriosis protocol is essential
Transvaginal ultrasound under the endometriosis protocol is the first line imaging investigation of choice
MRI under the endometriosis protocol provides essential additional detail for complex or deep infiltrating disease
Laparoscopy remains the gold standard for definitive diagnosis but should always be simultaneously therapeutic
Patient advocacy and knowledge are the most powerful tools in reducing diagnostic delay
The right diagnosis is not the end of the endometriosis journey — but it is the only place from which the right journey can begin.
